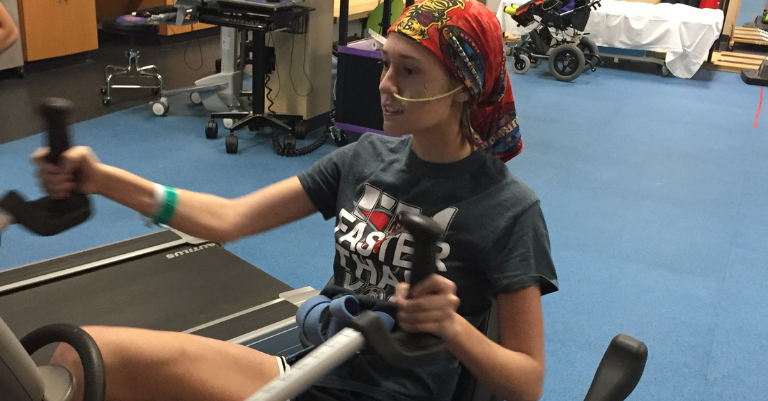
Physical therapy for traumatic brain injury (TBI) is a specialized rehabilitation approach that helps patients regain mobility, strength, balance, and functional independence after brain damage caused by external force. Whether you’re recovering from a mild traumatic brain injury like a concussion or navigating the complex challenges of severe traumatic brain injury, physical therapy will likely play a central role in restoring physical function and quality of life.
This guide covers tbi and physical therapy across all recovery stages, from acute hospital care through outpatient therapy and home-based programs.
After reading this article, you’ll understand:
- How traumatic brain injury affects physical abilities and why rehabilitation is essential
- Specific physical therapy approaches used at each recovery stage
- Methods for addressing common traumatic brain injury complications like spasticity and impaired balance
- How to navigate rehabilitation settings, from inpatient rehabilitation to home care
- Actionable steps for beginning your recovery journey with qualified health care providers
Understanding traumatic brain injury.
Traumatic brain injury (TBI) occurs when an external mechanical force disrupts normal brain function.1 TBI can result from motor vehicle accidents, falls, sports injuries, or penetrating head injuries that damage brain tissue directly. The location and extent of brain damage determine which physical symptoms emerge and how they affect daily functioning.
Brain injury disrupts the neural pathways controlling movement, balance, and coordination. A physical therapist specializing in neurological physical therapy understands how to work with the brain’s neuroplasticity (its ability to reorganize and create alternative pathways2) to restore lost functions or develop compensatory strategies.
Types and severity levels.
Traumatic brain injuries are classified by consciousness level, imaging findings, and symptom duration.
Mild traumatic brain injury (also known as a concussion) involves brief or no loss of consciousness, with symptoms typically resolving within weeks to months.3 Physical therapy for mild TBI focuses on gradual return to activity, vestibular therapy for dizziness, and cervical spine treatment for related neck dysfunction.
Moderate to severe TBI involves extended unconsciousness, significant cognitive impairment, and pronounced physical symptoms. Patients may emerge from a minimally conscious state requiring intensive rehabilitation. Severe traumatic brain injury often demands months of therapy to address profound motor deficits.
The severity of injury determines how patients will progress through the stages of brain injury recovery, as well as the course of treatment required. Mild cases may need only four to eight weeks of outpatient physical therapy, while severe injuries may require months of inpatient rehabilitation followed by extended community-based care.
Physical symptoms requiring therapy.
Brain injury can cause a range of physical symptoms, depending on which brain regions sustain damage. Such impairments include:
- Muscle weakness affecting one or both sides, difficulty initiating movements, or loss of fine motor control
- Impaired balance from vestibular dysfunction, inner ear damage, or disrupted sensory integration
- Difficulty sequencing movements, lack of muscle coordination (ataxia), or tremors during purposeful activity
- Muscle spasticity creating stiffness and abnormal posture, or flaccidity reducing functional strength
- Altered walking ability, asymmetrical gait patterns, or reduced endurance that limits mobility
The relationship between injury location and symptoms guides therapy selection. Frontal lobe damage, for example, often affects motor planning, while cerebellar injury disrupts coordination. Understanding these connections allows physical therapists to target interventions precisely.
It’s important to note that physical symptoms don’t exist in isolation, but rather interact with cognitive and emotional challenges, making an integrated approach to care essential for optimal outcomes.
Physical therapy approaches for TBI.
To support TBI patients through recovery, physical therapists apply evidence-based techniques. Each approach addresses specific functional limitations while building toward comprehensive recovery.
Motor function rehabilitation.
Restoring motor function after brain injury requires a structured approach that combines targeted strengthening with task-specific motor relearning. Physical therapy focuses on rebuilding strength, preserving joint mobility, and retraining movement patterns so patients can translate physical gains into functional independence. Interventions are sequenced to support safe, measurable progress toward everyday activities such as transfers, self-care, and mobility.
Strength training uses resistance training principles adapted for neurological populations. Parameters include specified frequency, intensity, and repetitions with appropriate warm-ups and cool-downs. Goals connect directly to functional outcomes—for example, hip strength for standing transfers or arm strength for self-care tasks.
Range-of-motion maintenance prevents joint contractures and muscle shortening from immobility. Interventions include passive exercises, proprioceptive neuromuscular facilitation (PNF) techniques, joint mobilizations, and positioning with splints or bracing. Maintaining flexibility ensures joints remain aligned for effective muscle recruitment during functional tasks.
Motor relearning emphasizes task-specific practice. Constraint-induced movement therapy (CIMT) forces use of an affected upper limb by restraining the unaffected side, overcoming learned non-use patterns. Studies show CIMT protocols of 6 hours daily for 2-3 weeks can produce significant improvement in arm function.4
Balance and coordination training.
Recovery of balance and coordination depends on both physical stability and the brain’s ability to interpret and integrate sensory input. Physical therapists target postural control, vestibular function, and coordinated movement through progressive, challenge-based training. As patients build stability, therapy advances from foundational alignment work to dynamic activities that mirror real-world demands.
Static balance training establishes fundamental stability through midline orientation and postural alignment exercises. Patients progress from supported sitting to unsupported standing, gradually reducing the base of support.
Dynamic balance training introduces movement challenges—weight shifts, reaching activities, responses to perturbations. Training on uneven surfaces like foam pads or incline boards simulates real-world conditions. Rhythmic stabilization techniques, where therapists apply resistance in multiple directions, evoke automatic postural adjustments more effectively than static holds alone.
Vestibular therapy specifically addresses inner ear-related dizziness and spatial disorientation common after head trauma. Balance exercises progress from stable surfaces to increasingly challenging environments.
Research on translingual neurostimulation (TLNS) combined with physical therapy shows promise for patients who plateau in balance recovery, demonstrating that adjunctive technologies may enhance outcomes beyond therapy alone.5
Functional movement training.
Functional training translates physical recovery into meaningful independence in daily life. Therapy emphasizes task-specific practice that rebuilds mobility, self-care skills, and safe navigation across environments. Interventions progress in complexity so patients can apply strength, balance, and coordination gains to real-world activities at home and in the community.
Gait training rebuilds walking ability through progressive challenge. Interventions include lower limb and trunk strengthening, sit-to-stand practice on varied surfaces, and dynamic balance on uneven supports. Progression reduces support levels and adds dual-tasking with cognitive elements to simulate community walking demands.
Activities of daily living training bridges physical abilities to practical function. Therapists work on bed mobility, transfers, dressing, and home navigation. For patients with severe TBI, wheelchair mobility training may precede walking goals.
Progression principles move from controlled environments to real-world complexity. Early training uses stable surfaces and single-task focus. Advanced training introduces variable surfaces, reduced bases of support (tandem stance, single-leg standing), and cognitive-physical dual-tasking.
Understanding these approaches sets the foundation for navigating the staged rehabilitation process.
TBI and physical therapy: Treatment stages and methods.
Physical therapy for TBI progresses through distinct stages, each with appropriate interventions and treatment plans. The rehabilitation continuum spans from hospital-based acute care through community reintegration, with intensity and focus shifting as recovery advances.
Acute stage interventions.
Immediate post-injury care establishes the foundation for later recovery. At this stage, physical therapy focuses on:
- Positioning and mobility: Therapeutic positioning prevents skin breakdown, respiratory complications, and joint contractures while the patient is immobile or minimally conscious.
- Respiratory support: Chest physical therapy maintains lung function during periods of reduced activity and altered consciousness.
- Preventing secondary complications: Early intervention addresses muscle stiffness, joint limitations, and circulatory issues before they become established.
- Early mobilization protocols: Research supports beginning physical activity as soon as patients are medically stable to optimize recovery timing while respecting acute inflammation windows.
During the acute care phase, physical therapists collaborate closely with physicians to determine safe activity progression based on blood pressure stability, intracranial pressure, and neurological status.
The rehabilitation process.
As patients stabilize medically, the focus of care shifts from preventing complications to rebuilding function and independence. At this point, therapy intensity, setting, and goals vary based on recovery needs, creating a structured progression across the rehabilitation continuum. The following comparison outlines how treatment approaches evolve from acute inpatient care through long-term rehabilitation and community reintegration.
Progression of care after traumatic brain injury.
| Key Considerations | Acute Inpatient | Sub-acute Rehabilitation | Outpatient Therapy | Home-Based Care |
| Treatment Setting | Hospital rehabilitation unit | Specialty hospital or residential facility | Clinic | Patient’s residence |
| Intensity Level | 3+ hours daily, multiple disciplines | 1-3 hours daily | 1-3 sessions weekly | Variable, often daily home exercises |
| Duration | 2-6 weeks | 3-6 months | Months to years | Ongoing maintenance |
| Typical Goals | Medical stability, basic mobility, sitting balance | Functional independence, walking, self-care, vocational training, community reintegration | Community reintegration, advanced skills | Maintenance, continued gains, family training |
Choosing the appropriate rehabilitation setting depends on the severity of the injury, medical stability, family resources, and insurance coverage. Severe TBI typically requires inpatient rehabilitation before transitioning to post-acute rehabilitation and eventually outpatient therapy.
For mild traumatic brain injury, outpatient or home-based physical therapy may be an appropriate first step.
Common challenges and solutions after TBI.
Patients recovering from a TBI encounter predictable obstacles that skilled intervention can address. Recognizing these challenges early allows therapists and families to implement solutions before progress stalls.
Spasticity and muscle stiffness.
Muscle spasticity (abnormally increased tone, creating stiffness and resistance to movement) is a common effect of moderate-to-severe TBI.
Solutions: Sustained stretching exercises reduce hypertonia through maintained muscle lengthening. Positioning programs using splints and serial bracing maintain joint range. Sensory modulation techniques such as maintained pressure (Lycra garments), slow stroking, neutral warmth, or prolonged cooling help normalize tone without medication. Physical therapists balance exercises that widen the base of support (which lowers tone) with activities that challenge stability. Severe cases may require botulinum toxin injections or other pain management approaches coordinated with healthcare provider teams.
Cognitive-physical integration issues.
Brain injury affects cognitive functions alongside physical abilities, creating challenges when therapy requires attention, memory, or problem-solving.
Solutions: Dual-task training deliberately combines physical and cognitive demands, starting simply and progressively growing more complex. Therapists simplify verbal instructions, use demonstration over explanation, and structure environments to reduce distractions. Occupational therapists often collaborate to address cognitive skills that support physical performance. Task breakdown presents complex movements as sequential steps rather than integrated wholes.
Plateaus in recovery progress.
Recovery often slows after rapid initial gains, which can be discouraging for patients and families.
Solutions: Advanced training techniques introduce novel challenges—new surfaces, different contexts, higher complexity demands. Equipment modifications like body-weight support treadmills or aquatic therapy change the training environment. Goal adjustment shifts focus to quality over quantity or redirects attention to previously unaddressed areas. Emerging approaches such as translingual neurostimulation show promise for patients with plateaued balance recovery—studies demonstrate gait and balance improvements beyond what physical therapy alone achieves. Sometimes, apparent plateaus actually reflect fatigue, requiring reduced intensity before advancing.
Recovery after a TBI is rarely linear, but with the right support, meaningful progress is possible at every stage. For more than 30 years, Nexus Health Systems has specialized in treating individuals with brain injury, stroke, and other complex neurological injuries and illnesses. In the Rise Program, we provide interdisciplinary care designed to help patients regain independence and prepare for the next level of care. If you or a loved one is navigating recovery after brain injury, our team is here to help you identify the right next step. Contact our admissions team to start the conversation.