Prader-Willi Syndrome (PWS) is a rare genetic disorder that affects learning and behavior resulting from an abnormality on the 15th chromosome. Individuals experience PWS differently and can have challenges, including health problems related to overeating and weight gain, delayed puberty, failure to thrive, compulsive, self-harm or aggressive behavior, and weakened muscle tone.
Like most children with PWS, Amber Woodworth experienced these challenges. Because her family didn’t know how to stop heading down the path they were on, they sought out help from specialists and Nexus Children’s Hospital.
“[Our daughter] would control everything we did,” said Amy Woodworth. “She was incredibly hostile towards me and her siblings and she would steal items from around the house and hoard them. I stopped talking to her or going into her room because I didn’t know if it would make her mad. She also gained a lot of weight — 75 pounds in just two years.”
According to the Prader-Willi Syndrome Association, a support organization for individuals and families, an estimated one in 12,000 to 15,000 people have PWS. Although there are many organizations around the country for adults with the syndrome, resources for young children and adolescents are few and far between. In fact, Nexus Children’s Hospital is the only facility in the country that has a program for children with PWS at this time.
Addressing comorbid medical issues and behavioral complications characteristic of individuals with PWS, the inpatient program helps young patients who have found traditional outpatient programs unsuccessful. Specific goals are set for every child regarding the following:
- Decreasing BMI
- Resolving weight-related conditions
- Developing strategies to manage behavior
- Developing strategies to decrease unstructured time
- Developing coping skills for home, school, and in the community
- Improving overall quality of life
The Jump Start Program incorporates low-calorie diets, set daily schedules, and individualized physical training regimens. While in the program, Amber lost 25 pounds and was evaluated for medicine to help her outbursts and anger. She also participated in daily activities that were part of a routine.
“I really had a good experience overall,” shared Amber. “We were always on walks, playing on the playground, or in the day room. I also think meeting my goals went really well.”
Behavioral health support is also available for both the patient and family members. Amy and Tim, Amber’s parents were involved in counseling as well, which Amy credits for her realization of the significance of their role in Amber’s progress.
“Dr. Cassidy and Dr. Leppo opened mine and my husband’s eyes to see that we needed to change,” explained Amy. “I wasn’t being consistent, and our home wasn’t safe because food was accessible and there wasn’t a lot of structure.”
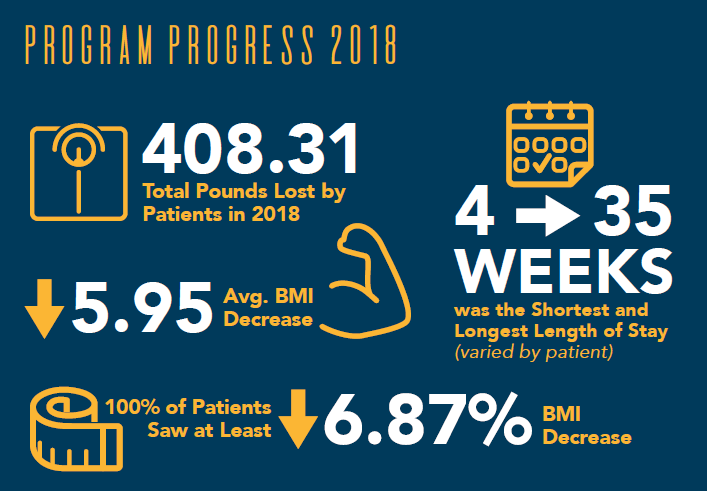
The inpatient program admits youth from three to twenty-one years of age from across the country since there is really nothing else available. This past year, dozens of youth benefited from the routine and activities, as was highlighted in our annual quality report: